When it comes to protecting our health, having a solid emergency plan is key—especially for those with weakened immune systems. Picture navigating through a crowded space filled with germs while knowing that your body needs extra help to stay healthy. For immunocompromised individuals, the stakes are higher, making infection control practices not just useful but essential. This article offers vital insights into creating an effective immunocompromised emergency plan, covering everything from risk assessments to recognizing symptoms early. By taking these proactive steps, individuals can significantly reduce their chances of falling ill and ensure they’re prepared in case an unexpected situation arises. Let’s dive into practical strategies that can make a genuine difference in keeping loved ones safe.
An immunocompromised emergency plan should include a thorough risk assessment, personal hygiene practices, and strategies for accessing medical care quickly. Additionally, it is essential to promote infection control methods such as hand hygiene, wearing masks in crowded environments, and maintaining a clean living space to minimize exposure to pathogens. Regular communication with healthcare providers for updated vaccinations and treatments is also crucial.
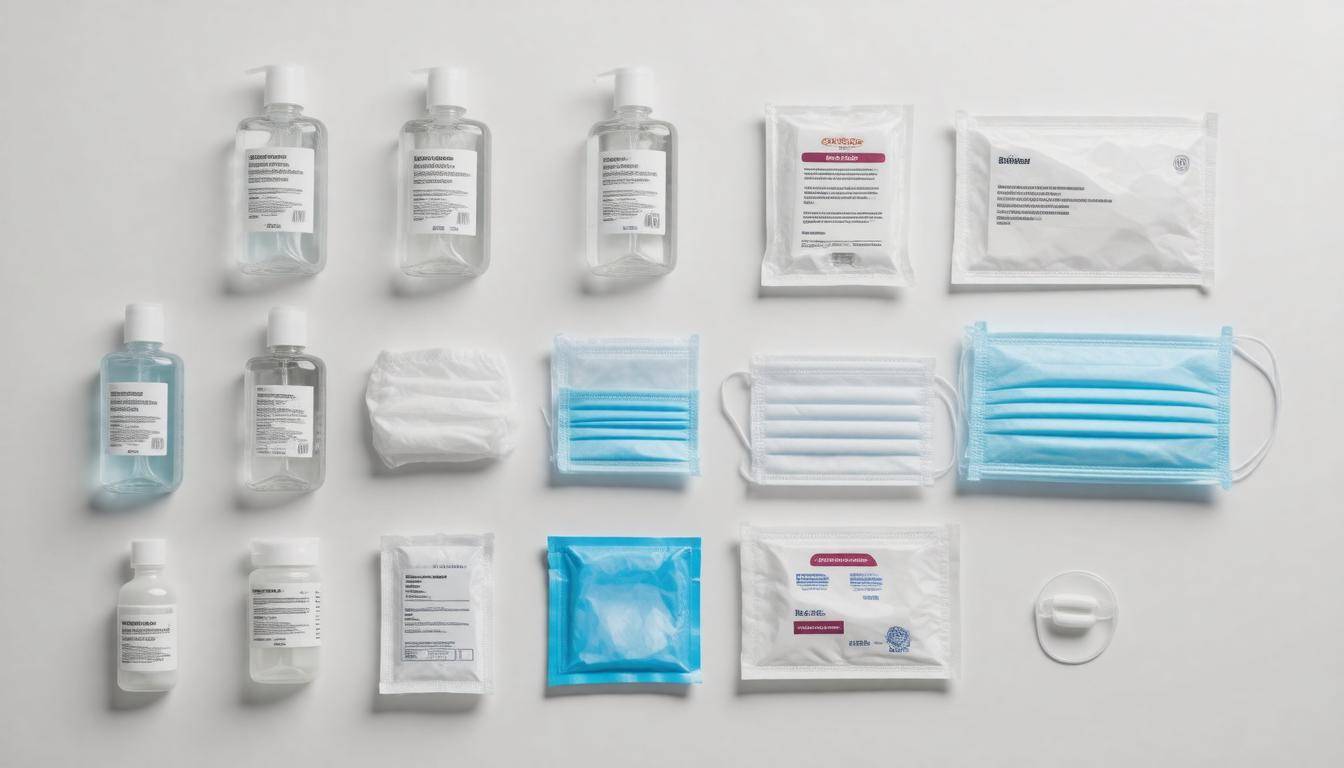
Immunocompromised Emergency Plan Summary
For individuals with compromised immune systems, having a well-structured emergency plan is not just advantageous—it’s essential. Such a plan serves as a roadmap to navigate various health challenges, especially in emergencies where access to medical care might be delayed or compromised. The plan must effectively address unique vulnerabilities by focusing on proactive measures that minimize exposure to pathogens.
Key Components of the Plan
-
Risk Assessment: The first step involves evaluating personal circumstances, lifestyle habits, and environmental factors that may pose infection risks. This includes understanding where illness may come from, whether it’s frequent visits to crowded places or exposure to sick family members.
-
Emergency Contacts: Creating a comprehensive list of emergency contacts is crucial. This should include healthcare providers familiar with the individual’s medical history, trusted family members who could assist in crises, and support groups that provide emotional and logistical assistance during trying times.
-
Essential Supplies: Having an accessible emergency supply kit is paramount for quick response during an emergency. This kit should contain necessary medications, hand sanitizers containing at least 60% alcohol for effective disinfection, masks to minimize virus transmission, and disposable gloves. Keeping all supplies organized in a designated place can save precious time when things get hectic.
-
Regular Check-ins: Scheduling frequent consultations with healthcare providers ensures that any changes in health status are monitored. During these appointments, the individual can review their emergency plan and make necessary adjustments based on current health needs or emerging threats.
By prioritizing these components, immunocompromised individuals empower themselves with tools to reduce their risk of infection.
Moreover, understanding the importance of keeping this plan dynamic is critical. As health conditions change, so too should the strategies put in place to mitigate risks. Regular updates with your healthcare team can aid in fine-tuning the approach while ensuring that new vaccinations or treatments are promptly integrated into the overall strategy.
Constructing an emergency plan requires ongoing attention and revision to adapt to both personal health changes and external circumstances such as seasonal outbreaks or health advisories from organizations like the CDC.
Essential Infection Control Precautions
Infection control should always be the foundation of any emergency plan designed for those who are immunocompromised. A good starting point is understanding that your surroundings play an immense role in your health. By establishing strict hygiene practices and being vigilant about possible pathways for infections, you can create a protective barrier against illness.
The significance of regular hand-washing cannot be overstated; washing your hands with soap and water for at least 20 seconds can drastically reduce the likelihood of infections, as it physically removes pathogens from your skin.
For example, imagine you’re stepping into your home after a long day out. Before you touch anything, you wash your hands to eliminate germs you’ve picked up along the way. This simple act can make a significant difference, especially when many illnesses spread through direct contact with contaminated surfaces or people.
Alcohol-based hand sanitizers serve as a reliable backup when soap and water aren’t readily available. A quick rub between the palms for at least 20 seconds ensures proper disinfection. Note that only products with at least 60% alcohol are effective.
It’s not just about your hands; routinely cleaning surfaces that frequently come into contact with hands—like doorknobs, light switches, mobile phones, and keyboards—is essential. Think of these surfaces as potential breeding grounds for germs. Setting aside time each day to wipe them down can dramatically reduce exposure.
Advanced Precautionary Measures
Another vital precaution involves wearing N95 masks, particularly in crowded or poorly ventilated areas. Imagine walking through a bustling grocery store filled with people—every breath taken carries the risk of inhaling airborne viruses. N95 masks have been shown to effectively block up to 95% of small respiratory particles, significantly lowering transmission rates. This just might be a game changer!
Take Sheila’s experience as an illustrative case: living with lupus means her immune system is compromised, causing her considerable concern over infections. Since she adopted strict mask-wearing protocols in public settings, she’s reported fewer instances of illness—even during peak flu season.
By adhering strictly to these protocols, you establish a safer environment for yourself and those around you. It’s about creating a protective network that decreases potential risks for everyone involved.
With infection control precautions in place, it becomes essential to discuss how community practices can further support overall health and well-being.
Community and Family Infection Guidelines

Family and community members play a pivotal role in creating an environment that inherently reduces the risk of infections for immunocompromised individuals. This involves more than just personal hygiene; it requires a collective effort to foster a culture of safety. Simple yet effective guidelines can significantly lower infection risk, making everyone feel safer in both the home and public areas.
Household Guidelines:
One of the most impactful practices is maintaining good personal hygiene within the household. Encouraging family members to wash their hands frequently—especially after returning home, before meals, and after using the restroom—helps minimize germs. Using hand sanitizers containing at least 60% alcohol will also contribute to reducing potential pathogens.
It might seem minor, but implementing a “no-shoes” policy inside the house can act like a gatekeeper against dirt and bacteria entering your living space. Think about how many surfaces your shoes come into contact with daily—it’s no wonder they can track in unpleasant germs.
Moreover, regular cleaning won’t hurt either. Disinfecting commonly touched surfaces like doorknobs, light switches, and countertops is vital. Establishing a weekly cleaning schedule can ensure these surfaces remain sanitized. A family responsibility chart might even make this task more engaging while encouraging everyone to participate.
Community Guidelines:
Extending these practices to community interactions is equally crucial. When you’re in public areas, staying vigilant and avoiding close contact with anyone displaying symptoms of illness is essential. This extends beyond just coughs and sneezes; subtle signs of discomfort or illness may suggest someone isn’t feeling well and could potentially spread infections.
Being aware of seasonal flu outbreaks can empower families to take proactive measures against illness. Subscribe to local health advisories or websites that provide updates on infectious disease trends within your area so you can be appropriately prepared and inform your loved ones as needed.
Taking precautions at home and in the community establishes necessary safeguards; understanding how to identify early symptoms serves as our next critical step in protecting ourselves and those we care about.
Recognizing Symptoms Early

Early detection of infections is non-negotiable when it comes to immunocompromised individuals. The sooner you recognize potential warning signs, the faster you can seek medical intervention. This proactive approach enhances recovery outcomes and safeguards against more severe complications down the road.
Common Symptoms to Watch For
-
Fever or Chills: A temperature above 100.4°F (38°C) is often one of the first indicators of infection. Many people may dismiss a slight fever, but for those with lowered immunity, it cannot be taken lightly.
-
Unexplained Fatigue: Feeling unusually tired? This is more than just a lack of sleep; it could signify an underlying infection demanding your attention.
-
Sore Throat or Persistent Cough: If you find yourself battling a persistent cough or soreness in your throat, these could signal respiratory infections that need evaluation.
-
Shortness of Breath: Difficulty breathing should never be overlooked. It may suggest an infection in your lungs and warrants immediate medical assistance.
-
Unusual Headaches: While headaches are common, those that come out of nowhere and feel different from your usual ones could signal trouble.
-
Changes in Skin Color or New Rashes: Pay attention to your skin; any new rashes or discoloration can indicate localized infections that require prompt care.
It’s worth noting that symptoms can appear anywhere from 2 to 14 days after exposure, varying based on the specific infection. This variability highlights the importance of vigilance—never hesitate to reach out to healthcare providers if you notice any concerning changes.
Recognizing early indicators is pivotal; however, addressing them appropriately is essential for effective risk mitigation during health emergencies.
Necessary Medical Steps
Immediate actions can play a pivotal role in how an infection progresses, especially for immunocompromised patients. When symptoms first appear, one of the most critical steps is contacting your healthcare provider. It’s essential to get on the phone as soon as possible. Make that call! Telehealth services are your friend here—they allow you to discuss your situation without leaving the safety of your home and minimize exposure risks.
During this initial conversation with your doctor, be ready to share specific details about your symptoms. Write them down if that makes it easier—focusing on the duration and severity can help your healthcare provider gauge how serious the situation might be. For example, if you’ve developed a fever or persistent cough, mentioning these symptoms will guide them in assessing the urgency of your care needs.
Once you’ve established communication with your healthcare provider, it’s time to follow through with their recommendations.
Step-by-Step Medical Actions
After reaching out to your doctor, follow any prescribed protocols diligently. If antiviral medications like Paxlovid or Remdesivir are indicated, starting treatment without hesitation is vital. Research shows that beginning antiviral therapy within five days of symptom onset can significantly reduce hospitalization risk by 87% for patients with mild to moderate COVID-19, particularly those who are unvaccinated.
Imagine you’re feeling feverish and achy; upon contacting your provider, they prescribe Paxlovid. You don’t delay—this decisiveness could very well determine the path of your recovery.
However, not all situations can be managed at home through telehealth consultations; some require immediate in-person evaluation.
In severe cases—like experiencing difficulty breathing or chest pain—heading straight to the Emergency Room (ER) becomes vital. Here’s where a few easy-to-follow precautions really matter: before you arrive, make sure to wear a mask to protect yourself and those around you. Inform the ER staff about your immunocompromised status at check-in so they can prepare for any specialized attention you may need.
Having clear communication and taking safety measures facilitates smoother care upon arrival and helps healthcare professionals provide appropriate treatment tailored specifically for you.
These medical steps highlight essential actions that can help in managing infections, setting the stage for understanding how different types of infections may require unique approaches.
Facing Specific Types of Infections
Not all infections are the same; indeed, they require tailored responses and treatment protocols. One common type of infection that poses a significant danger to immunocompromised patients is viral infections. These infections can spread easily and may cause devastating effects on those with weakened immune defenses. A key recommendation is to take antiviral medications as prescribed by healthcare professionals. For instance, Tamiflu is commonly utilized for mitigating symptoms associated with influenza, while Acyclovir serves as an effective treatment for herpes virus infections, preventing further outbreaks or complications.
However, we cannot overlook bacteria; these tiny invaders can wreak havoc on individuals whose immune systems are compromised.
When it comes to bacterial infections, relatively straightforward treatments become critically important. Antibiotics like Amoxicillin are frequently prescribed for bacterial pneumonia—a common yet serious concern for those with immunodeficiencies. It’s crucial that these antibiotics be taken exactly as directed and completed in their entirety, even if symptoms begin to improve. Failure to do so could lead to antibiotic resistance, rendering them ineffective in treating future infections.
Next, let’s explore the often underestimated realm of fungal infections which can turn life-threatening.
For immunocompromised individuals, the threat posed by fungal infections should not be underestimated. These infections can be particularly nasty and life-threatening; thus, prompt attention is crucial. It’s imperative that antifungal medications—such as Fluconazole—be utilized expediently after diagnosis. These medicines can make a significant difference in combating fungal pathogens that take advantage of weakened immune systems.
With these insights into the types of infections at hand, vigilance becomes vital for managing risks effectively.
Managing these infections requires both awareness and commitment from healthcare providers and patients alike. Early detection and appropriate intervention can significantly improve outcomes, ensuring those who are immunocompromised receive the care they need in a timely manner.
Moving forward, exploring available resources and support systems can dramatically enhance care strategies for this vulnerable population.
Resources and Support Networks
Having a robust support network can significantly enhance an immunocompromised person’s quality of life. Beyond just emotional support, these networks can provide valuable guidance regarding managing health risks associated with being immunocompromised. Imagine having a community that understands your struggles and offers practical advice—it makes facing everyday challenges much more manageable.
One effective avenue is joining online forums where patients come together to share experiences and resources. Websites like PatientsLikeMe allow individuals to connect over shared conditions, offering insights that can lead to better management strategies. Similarly, reaching out to organizations like the National Organization for Rare Disorders (NORD) can provide access to specialized knowledge tailored to rare conditions.
Julie, a patient with multiple sclerosis, realized the value of such networks when she found solace and vital information through a Facebook support group specifically for immunocompromised individuals. Her story illustrates how these connections can transform despair into hope, empowering members with practical tips and emotional encouragement.
| Organization | Resource Offered | Contact Info |
|---|---|---|
| CDC | Infection prevention guidelines | www.cdc.gov |
| NORD | Support groups and information on rare diseases | www.rarediseases.org |
| PatientsLikeMe | Online forums for patient support | www.patientslikeme.com |
| National MS Society | Resources for managing multiple sclerosis | www.nationalmssociety.org |
| Primary Immunodeficiency Foundation | Education and advocacy for immunodeficiency patients | www.primaryimmune.org |
Building these connections not only provides emotional support but also ensures access to essential resources that empower you to navigate health-related uncertainties effectively. Turning our focus now, we can examine the critical methods designed to maintain safety and care during potential health crises.
Effective Isolation Procedures
When someone in your household becomes infected, the importance of swift and efficient isolation cannot be overstated. The first step is to designate a specific room for the infected individual, ensuring that it is well-ventilated. This means cracking open a window when possible or using an air purifier to circulate fresh air. Keeping the environment breathable aids in minimizing viral load within that confined space, thereby reducing the potential for transmission to others.
Alongside creating a separate living space, use disposable utensils for meals. This eliminates the risk of shared items becoming vectors for spreading infection. If disposables aren’t available, ensure that all shared dishes are washed with hot, soapy water after each use—think of it as a protective measure akin to armor against contagion.
It’s also wise to set up a daily cleaning schedule for high-touch surfaces in common areas like doorknobs, countertops, and light switches. This regular disinfection is critical because viruses can linger on surfaces longer than people expect.
According to CDC guidelines, the recommended isolation period lasts between 7-10 days, but it’s always best practice to remain current with health advisories since recommendations can change based on emerging data.
It isn’t just about separating the infected person; it’s also about protecting their mental health during this uncertain time. Simple comforts such as regular video calls with family members outside of the isolation area can provide emotional support. Additionally, keep essentials like books, movies, or games available to help pass the time.
Caring for an infected individual safely requires clear communication with other household members about protocols and expectations. Everyone should understand that wearing a mask when entering shared spaces—however briefly—or venturing out is non-negotiable until the isolation period has concluded. It’s also beneficial to craft a chore schedule tailored to the needs of both those who are isolated and those providing care.
Lastly, personal hygiene practices cannot be overlooked. Ensure everyone in the household washes their hands regularly with soap and water for at least 20 seconds, especially after any interaction with the person who is ill. Hand sanitizers containing at least 60% alcohol can serve as an alternative when handwashing isn’t feasible but should complement—not replace—traditional washing.
By adhering to these effective isolation procedures, you’re not only managing the immediate infection but also fostering an environment of safety and care for all involved.
Maintaining vigilance during these challenging times is essential. Together, we can create a protective space that prioritizes health and well-being for everyone involved.
What role do caregivers play in an infection control plan for those who are immunocompromised?
Caregivers play a crucial role in the infection control plan for immunocompromised individuals by implementing hygiene practices, monitoring health status, and ensuring adherence to medical advice. They are responsible for creating a safe environment by minimizing exposure to pathogens, practicing hand hygiene, and administering medications as prescribed. Statistics show that effective caregiver involvement can reduce hospitalizations due to infections by up to 30%, showcasing their importance in preventing complications in vulnerable populations.
How should immunocompromised individuals communicate their needs to healthcare providers during an emergency?
Immunocompromised individuals should establish a clear and concise communication plan with healthcare providers, utilizing a designated medical alert card that outlines their condition, medications, and emergency contacts. Studies have shown that effective communication during emergencies can significantly improve health outcomes; for instance, a 2019 study found that patients who actively engaged in their healthcare planning reported a 30% reduction in adverse events. By proactively voicing their needs and preferences, immunocompromised persons ensure a swift response to their specific requirements, leading to better management of potential infections.
How can immunocompromised individuals best prepare their homes for infection control during a crisis?
Immunocompromised individuals can best prepare their homes for infection control during a crisis by creating a clean and safe environment: regularly disinfect high-touch surfaces, maintain good ventilation, and establish a designated area for medical supplies. According to the CDC, regular cleaning can reduce the risk of infections by up to 95%. Additionally, stocking essential items such as hand sanitizers, masks, and personal protective equipment is crucial in preventing exposure to pathogens during emergencies. It’s also important to limit visitors and ensure that those who enter the home practice proper hygiene protocols.
Are there any recommended resources or guidelines for creating an effective emergency infection control plan?
Yes, there are several recommended resources for creating an effective emergency infection control plan. The Centers for Disease Control and Prevention (CDC) provides comprehensive guidelines on infection control practices, especially for vulnerable populations such as the immunocompromised. The World Health Organization (WHO) also offers valuable resources, emphasizing the importance of hand hygiene and isolation protocols. In fact, implementing these guidelines can reduce healthcare-associated infections by up to 70%, making them essential for protecting at-risk individuals during emergencies.
What specific infections pose the greatest risk to immunocompromised individuals during emergencies?
Immunocompromised individuals face heightened risks from various infections, particularly opportunistic pathogens like Pneumocystis jirovecii, which can lead to pneumonia, and cytomegalovirus (CMV), known for causing severe complications. According to the Centers for Disease Control and Prevention (CDC), approximately 20-30% of people with weakened immune systems may develop infections from these pathogens during emergencies, underscoring the importance of strict infection control measures in crisis situations. Other notable threats include invasive fungal infections and bacterial sepsis, necessitating vigilant monitoring and proactive healthcare interventions.
