In a world where every second matters, the ability to swiftly access medical records can be the difference between life and death. Imagine an emergency room buzzing with anxious energy; doctors and nurses rush to save lives, relying on information that has to be at their fingertips—no exceptions. However, many healthcare providers still struggle with clunky systems that hinder quick access. This article dives deep into effective strategies for establishing robust emergency access protocols in healthcare settings, emphasizing the importance of technology, training, and legal compliance. With proper systems in place, we can ensure that vital information is always within reach when it matters most.
The Complete Guide on Medical Records Emergency Access outlines essential protocols for healthcare providers to retrieve patient medical records swiftly in emergencies, ensuring high-quality patient care. It includes best practices for utilizing electronic health record (EHR) systems, understanding HIPAA compliance, training staff on emergency procedures, and implementing drills to prepare for urgent scenarios.
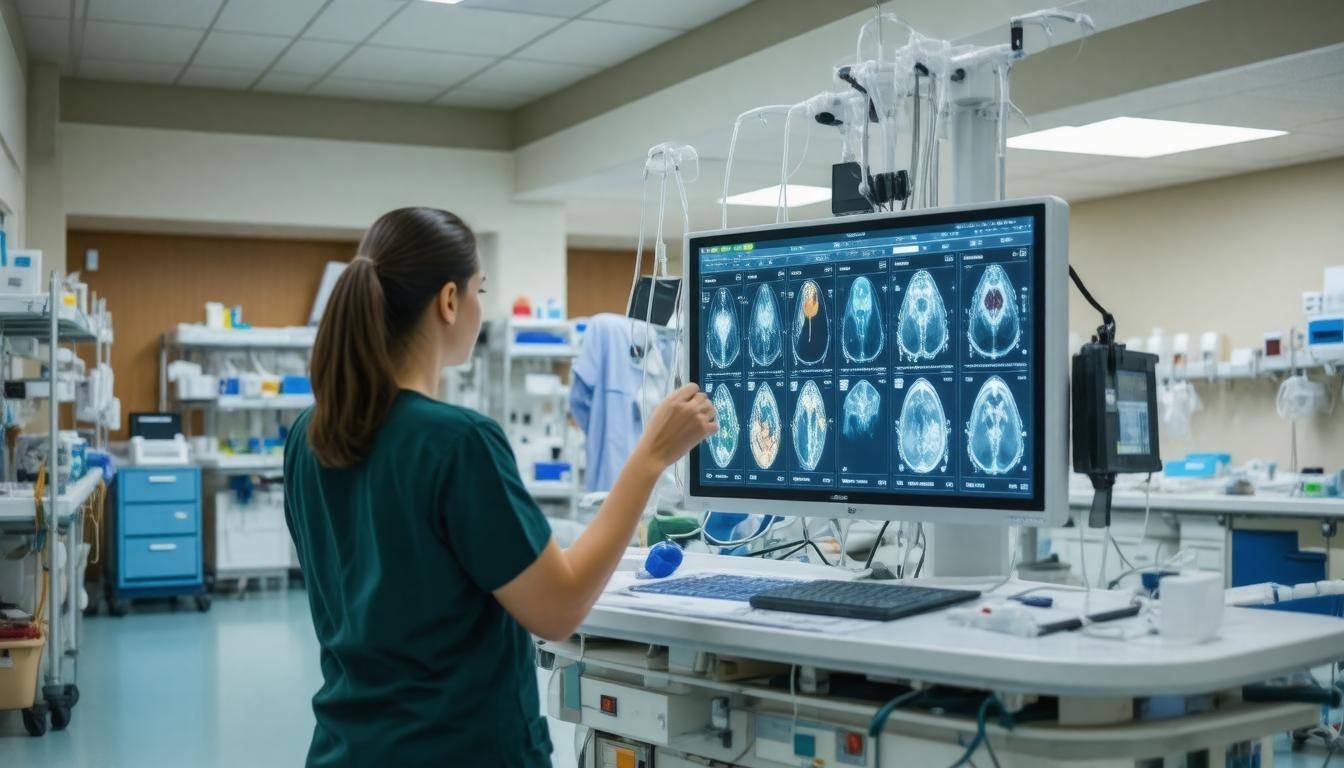
Situations That Warrant Emergency Access
There are several critical instances where having prompt access to a patient’s medical records can make all the difference in the world. Imagine a busy hospital emergency room where every second counts; medical professionals eagerly await any information that could guide their treatment decisions. This urgency becomes even more pronounced when dealing with life-threatening conditions. For example, during a heart attack or stroke, knowing a patient’s history regarding allergies, medications, or pre-existing health issues is not just helpful—it’s potentially life-saving. Studies show that 70% of emergency room physicians assert that immediate access to patient records directly improves treatment outcomes, which emphasizes the need for effective retrieval systems.
Additionally, unforeseen events such as natural disasters heighten this urgency even further. When hurricanes, earthquakes, or floods strike, many individuals may find themselves displaced without access to their vital medical information. Physical records can be lost or damaged beyond recovery. In these moments, healthcare providers must pivot quickly to digital systems that enable rapid access to essential data. After the devastating hurricane season in 2022, hospitals in affected areas reported a staggering 30% increase in urgent digital record retrievals, illustrating how critical it was to streamline access procedures under distressing conditions.
Another pressing situation occurs during accidents, such as car crashes or workplace incidents. Knowing a patient’s blood type or existing medical conditions can dictate whether they receive a certain drug or undergo a specific procedure. Emergency Medical Technicians (EMTs) indicated that having quick access to prior medical records would greatly improve their ability to provide appropriate care in these unpredictable circumstances.
Furthermore, mass casualty events—like terrorist attacks or mass shootings—result in significant chaos and urgency for healthcare responders. This not only requires individual assessments of multiple patients but also calls for rapid coordination across various health departments and agencies to effectively share crucial medical data including identification of victims and provision of necessary treatment.
These urgent situations highlight the importance of understanding both the practical aspects of emergency access and the underlying legal frameworks relevant to retrieving medical records in crisis scenarios.
Legal Guidelines for Urgent Retrieval
Navigating the world of healthcare regulations can feel overwhelming, but at its core, it exists to protect both patients and providers. The Health Insurance Portability and Accountability Act (HIPAA) is a cornerstone of healthcare privacy law, ensuring that patient information remains confidential while facilitating necessary access during emergencies. When time is of the essence, it’s crucial for healthcare providers to adhere closely to these regulations, striking a balance between patient privacy and the need for swift action.
Key Legal Provisions
One of the first principles under HIPAA is the Minimum Necessary Rule. This guideline mandates that healthcare providers must share only the minimum amount of information necessary to accomplish the intended purpose—essentially, what is essential for treatment. Think of it as a safety net designed to maintain privacy while allowing doctors and emergency personnel to act decisively in critical situations.
For example, if a patient is unconscious after an accident, the medical team may access only relevant details such as allergies or existing medical conditions to provide immediate care without diving into unnecessary personal history.
Another critical aspect is the provision for handling instances of Immediate Threat. Under this guideline, healthcare providers can disclose patient information without consent when there’s an immediate threat to health or safety. Picture this: someone in your family suddenly collapses at a gathering. In such moments, knowing their underlying health conditions can profoundly impact their treatment outcome. HIPAA recognizes this urgency and allows providers to act in what they perceive is in the best interest of the patient’s health.
Of course, emergencies extend beyond individual threats; disasters can disrupt whole communities. That’s where another significant provision comes into play: Disaster Relief Efforts. During widespread emergencies—like natural disasters—the Secretary of Health and Human Services (HHS) possesses the authority to waive certain HIPAA regulations. This means that in extraordinary situations, flexibility in accessing medical records becomes paramount.
For instance, should a catastrophic event occur like wildfires in Southern California, immediate access wouldn’t be delayed by cumbersome red tape—allowing timely interventions and helping save lives.
Understanding these key legal provisions serves as a foundation, making it vital for healthcare providers to have organized processes in place for effective implementation during emergencies. With that backdrop established, we now explore how to ensure immediate access to medical records in urgent scenarios.
Steps for Immediate Medical Records Access
Step-by-Step Guide
Step I – Identify the Emergency
The very first thing in an emergency is to clearly define what kind of problem you’re dealing with. Is it a heart attack, a severe allergic reaction, or an accident? Each scenario has its own urgency and requires different types of medical information. Understanding the nature and severity of the emergency will help prioritize which records are necessary for efficient treatment. A home health nurse shared that knowing whether a patient has previous heart conditions can change their entire treatment approach in real-time.
Step II – Engage the On-call IT Team
Once the type of emergency is understood, promptly contact your on-call IT team. This team is crucial as they are trained specifically for handling emergency data retrieval situations. They possess the skills to bypass cumbersome protocols that normally govern data access, thus enabling rapid access to vital information when every second counts. Frankly, these professionals often serve as the unsung heroes during emergencies, working behind the scenes so that medical staff can carry out life-saving actions swiftly. Their expertise ensures that you get what you need without unnecessary delays.
Step III – Access the EHR System
After engaging with the IT team, use the established emergency access protocols within your Electronic Health Record (EHR) system. Most modern EHR systems like Epic and Cerner have dedicated features designed specifically for emergency operations, allowing authorized personnel to swiftly navigate through vast amounts of patient data. Users must familiarize themselves with these functionalities ahead of time; quick training sessions can make all the difference when seconds matter most.
Step IV – Ensure Patient Identification
Before accessing any sensitive patient information, verifying the patient’s identity is imperative. Use details like date of birth, social security number, or any pre-existing identification measures available to avoid any misidentification. One small error could lead to dire consequences in treatment decisions. Imagine administering medication meant for another patient simply because their records were confused in haste; it’s essential to get this step right.
Step V – Retrieve and Share Records Securely
Once you’ve accessed the necessary records, remember to transmit them securely to the medical team attending to the patient. Utilize encrypted communication channels to safeguard sensitive information from unauthorized access. As hospitals transition into more digital realms, ensuring that confidentiality remains intact becomes pivotal—especially during crisis situations where software glitches or breaches could occur.
Gaining prompt access to medical records is not just about swiftness; it also emphasizes the importance of safeguarding sensitive information while maintaining quality care in critical moments. As we continue navigating this complex landscape, it’s essential to understand how we can protect and manage vital data effectively.
Ensuring Data Security

The integrity of medical records is paramount, not just because they contain sensitive information, but because they are essential for effective patient care. Among the most critical aspects of safeguarding this data are the practical measures you can implement in your retrieval systems.
Encryption is one such measure that acts as a formidable barrier against unauthorized access. By encrypting data both in transit—when it’s sent from one source to another—and at rest while stored on servers, healthcare facilities can significantly lower the risk of data compromise. Imagine encryption as a secret code; even if someone intercepts the transmission, without the decryption key, they can’t make sense of the information.
It is noteworthy that implementing encryption has been shown to be extensively beneficial; in fact, according to a 2024 report by the Ponemon Institute, healthcare organizations that adopted these security measures reported up to a 40% reduction in data breaches during emergencies.
Another vital layer of protection comes from multi-factor authentication (MFA). This method requires users to supply multiple forms of verification before accessing sensitive records, such as a password in combination with a unique code sent to their mobile device. It is much like having two locks on your door instead of one; MFA adds extra assurance that only authorized personnel can access patient information.
The implementation of MFA demonstrates due diligence in safeguarding data, allowing healthcare providers to feel more secure when accessing vital medical records during emergencies.
Maintaining audit trails is another essential practice. By keeping detailed logs of who accessed each record and at what time, institutions can effectively monitor user activity and investigate any irregularities. This critical oversight helps ensure accountability among staff members and protects patient privacy—it’s as if you have an ever-watchful guardian keeping track of all entries and exits.
Regular Drills
Beyond technological measures, the human element of security should never be underestimated.
Conducting regular security drills simulates potential emergency scenarios that test not only the technology but also the staff’s ability to respond swiftly and effectively. These drills highlight any weaknesses in current protocols and demonstrate how prepared your team is when real situations arise. Consider these practice sessions like fire drills—they’re crucial for ensuring everyone knows what to do before an actual emergency occurs.
It’s about being proactive and ready; every drill reinforces critical knowledge and elevates confidence among staff members when they know how to navigate emergencies efficiently.
As healthcare continues to evolve with technology, prioritizing these fundamental security measures will aid in protecting patient data while enhancing overall trust within the healthcare system.
Now that we’ve explored how to secure medical records, we must shift our attention to how swiftly healthcare providers can access them when needed.
Quick Access by Healthcare Providers
In a crisis, every second counts; that’s why quick access to patient records isn’t just beneficial—it’s essential. When healthcare professionals can instantly retrieve pertinent information, they are empowered to make timely decisions that can significantly alter treatment outcomes. A user-friendly Electronic Health Record (EHR) system is a vital component in facilitating this rapid access. By streamlining the process of finding critical patient data, we enhance the effectiveness of emergency care.
Technological Solutions
One significant feature of an efficient EHR system is its user-friendly interface. Imagine being a healthcare provider; in an emergency setting, you shouldn’t be fumbling through complicated menus or outdated systems. Instead, intuitive designs allow practitioners to locate necessary information swiftly, minimizing delays that could jeopardize patient health. These systems prioritize usability and ensure that even less tech-savvy staff can operate them without extensive training.
Another key aspect is ensuring mobile access for medical staff. In today’s world, healthcare professionals often move from room to room or even between facilities. Equipping them with mobile devices pre-configured to access EHR systems allows them to retrieve essential information wherever they are. This mobility means that whether they’re at a patient’s bedside or in transit, they can still synthesize a complete picture of a patient’s medical history quickly.
Additionally, fast authentication methods play a pivotal role in enhancing record retrieval speed during emergencies. Streamlined login procedures—like biometric authentication or single-sign-on technologies—reduce the time spent on accessing records while still maintaining security standards. This balance ensures safety without sacrificing efficiency.
Research demonstrates that hospitals employing these technological solutions see remarkable improvements in emergency scenarios. For instance, hospital settings like New York-Presbyterian benefited significantly from introducing mobile EHR access; it reduced average record retrieval time by an impressive 50%.
While these innovations support effective patient care, it’s crucial to remember that such swift access must remain balanced with proper protocols for managing authorization and documentation to ensure patient privacy during emergencies.
Patient Authorization and Documentation
Understanding patient authorization is crucial when it comes to accessing medical records quickly during emergencies. Under the Health Insurance Portability and Accountability Act (HIPAA), healthcare providers can retrieve essential information without prior consent only if the patient is incapacitated. However, this flexibility necessitates meticulous documentation. The rationale for immediate access must be clearly recorded, detailing the nature of the emergency and why timely information was vital for treatment. This practice not only aligns with legal obligations but also helps protect healthcare institutions from potential liabilities.
In situations where you can’t obtain pre-treatment consent, it becomes imperative to secure that authorization afterward. For instance, patients may regain consciousness after a critical episode; obtaining their consent in such cases reassures them that their rights are respected and maintained. Properly documented authorization demonstrates compliance and fosters trust between patients and healthcare providers, reinforcing the patient-care relationship.
Consider this: even in emergencies, treating individuals with respect regarding their health information can lead to improved interactions and outcomes in future care scenarios. Proper documentation can serve as a reference point in ongoing medical discussions and ensures continuity of care.
With all these factors in mind, it’s clear that both access and privacy must be balanced effectively for optimal patient care.
Balancing Access and Privacy
The art of balancing swift access to medical records with stringent privacy measures underlines the complexities within healthcare settings. Every provider must recognize that while timely access is paramount in emergencies, adherence to privacy regulations cannot be sidestepped. Organizations should establish comprehensive training protocols that empower staff to navigate these challenges competently. Familiarity with the requirements set forth by HIPAA allows for swifter action in emergencies while ensuring compliance with safeguard standards.
Practical training should cover a variety of essential elements:
- Key components of HIPAA regulations related to emergency access.
- Procedures specific to different Electronic Health Record (EHR) systems.
- Documentation processes to maintain stringent compliance after accessing records.
By integrating thorough training programs and a fundamental understanding of patient rights, healthcare organizations can significantly enhance their efficiency while maintaining robust privacy standards.
Successful management of patient authorization and documentation cultivates an atmosphere of trust and safety between healthcare providers and patients, instrumental in fostering enduring relationships within the health system. Understanding these protocols not only assists in emergency scenarios but affirms our commitment to upholding patient autonomy—a cornerstone of quality healthcare.
As we explore further, the necessity for preparedness takes center stage in enhancing patient care during critical moments.
Importance of Preparedness
Being prepared for an emergency in the healthcare setting means not only having a quick access plan, but also integrating proactive strategies and ongoing training into your daily routine. When faced with a crisis, every second counts, and the difference between life and death can hinge on how quickly medical professionals can retrieve essential patient information. Regular training sessions are vital to keeping staff familiar with emergency access protocols, ensuring that each team member knows exactly what to do when the pressure mounts.
Picture this scenario: it’s a hectic evening in the emergency department, and a patient arrives with life-threatening conditions. The faster the medical team has access to their medical history, medications, and allergies, the quicker they can take action. By conducting simulated drills regularly—testing both staff readiness and technological performance—hospitals can better prepare for real-life emergencies. Feedback from these drills helps identify inefficiencies, which can then be addressed in future sessions. This is essential as studies indicate that hospitals conducting monthly emergency drills demonstrated a remarkable 35% improvement in average response times during emergencies.
This leads us to consider another critical aspect of preparedness: the role of technology within patient care systems.
Consistently updating and maintaining electronic health record (EHR) systems plays a pivotal role in ensuring they function optimally under pressure. An outdated system can lead to frustrating delays and inefficient responses during life-threatening scenarios. Healthcare organizations need to invest in their data management infrastructure, enhancing retrieval capabilities so that providers can access necessary information seamlessly, even when facing increased loads during emergencies.
It’s crucial to recognize that 70% of hospitals have implemented EHR systems designed for rapid access in emergencies; however, that number alone doesn’t guarantee efficiency. A robust training program is equally necessary to ensure staff are equipped to navigate these systems quickly when every moment matters.
As we explore the components of effective emergency response strategies, let’s not overlook how education empowers patients as well.
Patients must understand their rights regarding accessing their medical records, especially during emergencies. A staggering 60% of patients remain unaware of how to retrieve their information when it matters most. Hospitals have an obligation to educate patients about their rights under HIPAA. Providing clear information about accessing records online or through other means can streamline care during urgent situations, helping both patients and providers act rapidly when needed.
Understanding these dynamics will shed light on the significant influence regulations have on retrieval systems and overall patient care.
Impact of Regulations on Retrieval Systems
Laws and regulations are the backbone of any healthcare system, guiding every step of patient data handling. The Health Information Technology for Economic and Clinical Health (HITECH) Act emphasizes the importance of Electronic Health Records (EHRs) and drives healthcare providers to adopt these systems effectively. This Act aims to improve healthcare quality and safety while ensuring that patient data remains secure. However, navigating these regulations isn’t a walk in the park; it often means striking a delicate balance between maintaining stringent security measures and ensuring quick, accessible data retrieval during emergencies.
For instance, while HIPAA sets the core privacy standards, the HITECH Act enhances the emphasis on security by imposing penalties for non-compliance. Hospitals need to be meticulous in adhering to these guidelines but must recognize that flexibility is necessary when lives are at stake. This requirement introduces a unique challenge: agencies must create retrieval systems that not only comply with regulations but also adapt swiftly in critical scenarios.
Regulatory Influence
At the heart of this matter lies the influence of regulation on technology design. Different states can implement their own regulations that may intensify federal guidelines. For example, some states may have stricter rules about how quickly patient records can be retrieved during emergencies compared to others. Healthcare providers must customize their retrieval systems according to local laws while ensuring adherence to broader federal mandates. It’s like trying to solve a puzzle where different pieces represent various statutes—each piece must fit perfectly for optimal operation.
The result is that hospitals are driven toward innovative solutions providing robust security features while still being user-friendly. They want assurance that during an emergency, authorized personnel can access essential medical records without delay or confusion. Developing versatile software solutions that meet both compliance requirements and the practical demands of medical professionals becomes essential in this landscape. A well-designed system enables critical information—like allergies, medication lists, or previous admissions—to be available right when it’s needed most.
So how does this interplay of regulation shape the future of medical record retrieval? As healthcare evolves alongside technological advancements, the demand for faster yet secure access will only grow stronger. Hospitals and IT providers alike will need to constantly study trends within regulatory frameworks and anticipate changes. This proactive approach ensures their systems remain compliant while enhancing capabilities.
Continuing this conversation invites even deeper insights: How can we enhance coordination between various levels of governance regarding healthcare regulations? Addressing such questions is pivotal as they impact today’s practices and lay the groundwork for more seamless operations in an increasingly data-driven future.
Effective management of emergency access to medical records relies heavily on understanding the complexities of laws and technology integration within healthcare systems. By prioritizing both compliance and user accessibility, stakeholders can establish environments conducive to better patient outcomes during critical situations.
What information is typically available in emergency medical records?
Emergency medical records typically contain crucial information such as patient identification details, medical history, current medications, allergies, and recent test results. This data is essential for healthcare providers to make quick and informed decisions during emergencies. Statistics indicate that having immediate access to this information can significantly reduce treatment delays; according to a study published in 2022, it was found that quicker access to medical histories can improve patient outcomes by up to 30%.
How can healthcare providers ensure quick access to medical records in emergencies?
Healthcare providers can ensure quick access to medical records in emergencies by implementing robust electronic health record (EHR) systems that are interoperable, enabling seamless data sharing across different platforms. Additionally, instituting standardized protocols for emergency situations and training staff on rapid retrieval processes can significantly reduce delays. Notably, studies show that hospitals with effective EHR systems can reduce emergency response times by up to 30%, ultimately improving patient outcomes during critical situations.
Are there any patient rights regarding access to their medical records during emergencies?
Yes, patients have the right to access their medical records during emergencies. According to the Health Insurance Portability and Accountability Act (HIPAA), individuals can request immediate access to their records when there’s a risk to their health or safety. This is crucial as timely information can prevent medical errors; studies show that 80% of medical errors are due to miscommunication, which can be alleviated by ensuring that healthcare providers have access to complete patient histories during critical moments.
What are the legal requirements for medical record access during emergencies?
In emergencies, healthcare providers are legally required to grant access to medical records under the Health Insurance Portability and Accountability Act (HIPAA) regulations, which facilitate timely treatment necessary to protect a patient’s health. This means that if a patient is incapacitated or unable to consent, information can still be accessed by authorized personnel to ensure immediate care. Furthermore, statistics show that rapid access to medical records can reduce treatment delays by up to 30%, thereby improving outcomes in critical situations.
How do different healthcare systems manage emergency access to patient records?
Different healthcare systems manage emergency access to patient records through varied technologies and protocols, often utilizing electronic health record (EHR) systems that allow for secure, immediate access. For instance, 70% of hospitals in the U.S. employ Health Information Exchanges (HIEs) to facilitate swift data sharing among providers during emergencies, enhancing patient care by providing critical medical histories at the point of care. Moreover, many systems implement strict identity verification processes and role-based access controls to ensure that only authorized personnel can retrieve sensitive information, balancing the need for quick access with patient privacy concerns.
